
A Community Approach to Health
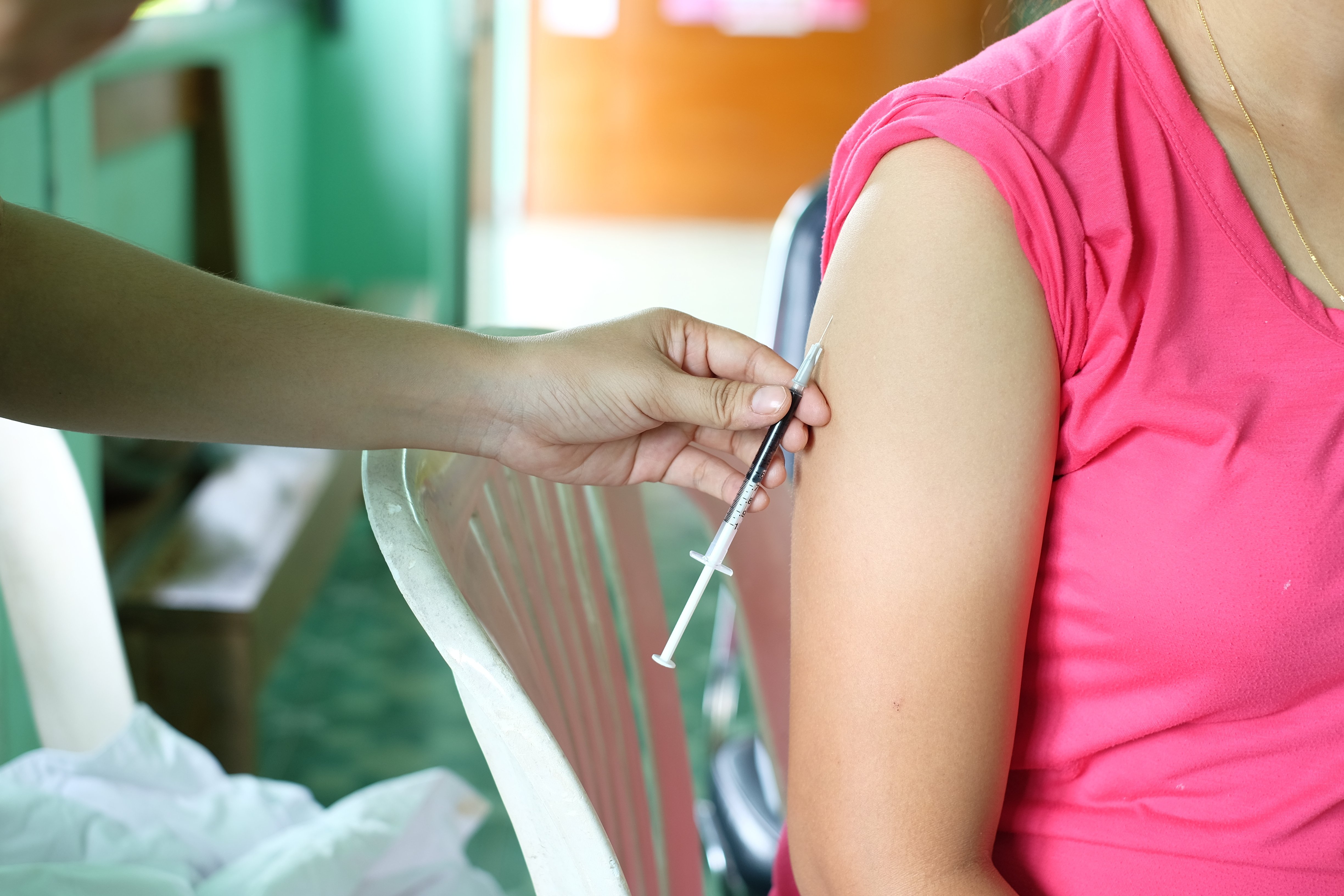
Sometimes,
pushing mandatory vaccination laws through governing bodies may not be the best
way to reach the human bodies they’re intended to influence.
Take
California’s new law,
which has catalyzed a wave of opposition from thousands of state residents.
Protestors have been mobilizing, and California’s secretary of state approved
an initiative allowing opponents of the bill to gather petition signatures
in the hopes of reversing the immunization bill through a referendum vote.
State Senator Richard Pan, the pediatrician who authored the bill, has received death threats
and may even face a recall election, which might push him out of office.
California’s
law—which abolishes exemptions from vaccines for personal beliefs rather than
medical necessity—is a good thing. Still, the intense public backlash to it
makes it plain that the law is neither popular nor safe from repeal.
Dan
Salmon, Deputy Director of the Institute for Vaccine Safety at Johns Hopkins
Bloomberg School of Public Health, told me in an interview that he’s concerned
the law will backfire. He recommends that states considering similar
legislation wait to see what happens in California before taking further
action.
While
Salmon supports efforts to make vaccine exemption laws more stringent, he
recently wrote
that “getting rid of non-medical exemptions altogether
and making mandatory vaccination truly compulsory risks substantial public
backlash and could be counterproductive to the ultimate objective of reaching
and sustaining high rates of [immunization] coverage and disease control.”
In
general, anti-vaxxers oppose
immunization legislation that constrains what they see as their individual
right to choose how they go about being parents.
And
here’s the crux of the problem. When it comes down to it, vaccines are about
community, not individuals. Pathogens and the diseases they spread defy our
best attempts to define ourselves as singular persons existing in the world as
individuals. They remind us that as much as we try to deny it, we are organisms
living in a web of organisms, hopelessly, and wonderfully, interconnected. The
more we continue to use the rhetoric of individual choice—whether to affirm or
combat required vaccinations—the more we lose the thread of why vaccines are
one of the backbones of public health.
When
a large enough portion of the population is vaccinated against a disease, the
phenomenon known as herd
immunity prevents outbreaks and protects those who don’t have personal
immunity from the illness. Many people have weakened immune systems and are
medically unable to be vaccinated. At the heart of the concept of herd immunity
must be a society’s commitment to protecting the most vulnerable: the lung
transplant recipients, the cancer patients, the infants,
and the pregnant mothers.
In
her book On Immunity, writer Eula Biss emphasizes
the connection between vaccine hesitancy and the
misconception that the decision to vaccinate is an isolated individual choice.
Biss writes, “When I asked a friend how she would feel if her child contracted
an infectious disease and did not suffer from it but passed it to someone more
vulnerable who would suffer, she looked at me in surprise. She had not, she
told me, considered that possibility.”
Biss
reveals that vaccine-hesitant mothers (which she was herself prior to writing On Immunity) –married, college-educated,
relatively wealthy, white women – generally distrust the government and the
pharmaceutical industry. My own research found that even when controlling for
education, race, and socioeconomic status, parents who distrust
the government and healthcare professionals are less likely to vaccinate their
children and more likely to view information about immunizations from
government agencies through a lens coated with skepticism and suspicion.
If
we can stop talking about immunizations solely in the realm of individual
choice and understand them as an essential part of being a part of a community,
maybe we can work toward finding solutions that are guided by togetherness,
empathy, and a sense of purpose, rather than through policies that opponents
view as paternalistic. Perhaps we can change the dynamic to embrace more
community-driven efforts to educate and mobilize on behalf of vaccines.
For
instance, what if rather than relying on preachy pamphlets on “Why you should
vaccinate” or harried pediatricians rushing to get to the next patient to
convey the message about vaccines, we tapped other parents in the community to
communicate with vaccine-hesitant parents?
Parent-to-parent
communication is one of the guiding principles at Voices for Vaccines,
a parent-driven organization that educates other parents about
immunizations. The same way that parents advise one another on what diapers to
choose and what preschools have the best teachers, Voices for Vaccines empowers
parents who vaccinate to reach out to vaccine-hesitant parents to share stories
about why they vaccinated their children.
It
is essential that hesitant parents are reached as early as possible by peers
with evidence-based experience, rather than friends who reinforce their
skepticism. Karen Ernst, one of two young mothers who re-launched Voices for
Vaccines in 2013, says that most parents make their vaccinating decisions long
before seeing their pediatrician. “By the time their ears have been filled with
their friends’ stories, a five-minute conversation with a doctor is not enough
to replace bad information with good,” Ernst explained in an interview.
“Parent
advocates are in a unique position to inoculate their friends and family
members against that bad information so that when they head into the doctor’s
office, they already feel confident about a medical decision that should be a
given,” said Ernst.
Mobilizing
the majority of parents who do immunize their children to see vaccine hesitancy
as a legitimate problem has been a challenge Voices for Vaccines has fought to
overcome. Despite recent events like the Disneyland
measles outbreak, even parents who believe everyone
should vaccinate “are complacent because the diseases we vaccinate against are
so rare. They do not understand that outbreaks like the one that began in
Disneyland late last year are canaries in the coal mine.”
For
his part, Salmon is interested in the prospects of parent-to-parent communication
but cautions that while the method has “much potential,” as of yet there is
little data or analysis that attests to its efficacy. In other words, as
lawmakers and thought leaders consider changing their rhetoric, they might also
want to start filling this gap in the research.
Grassroots
organizations like Voices for Vaccines that generate a healthy dose of positive
peer pressure could help increase vaccination rates in California and
elsewhere, where immunizations have become a flashpoint of fundamental
liberties. Parent-to-parent communication won’t be a panacea for vaccine
hesitancy, but it could be a step away from reifying immunizations as an
epicenter of individual choice and toward viewing them more accurately as a
commitment to common humanity.



