Table of Contents
- Executive Summary
- Preface: Why We Need Good Policy and Good Implementation of Public Paid Family and Medical Leave programs
- Research Process
- Key Learnings
- Learnings Part 1: Communicating Effectively about PFML
- Learnings Part 2: Outreach
- Learnings Part 3: Applications, Processing, and Delivery
- Learnings Part 4: IT Infrastructure and Culture
- Conclusion
- Additional Resources
Learnings Part 3: Applications, Processing, and Delivery
3.1. Conceptual and Cultural Considerations
3.1.1 Set Realistic Expectations and be Transparent
3.1.2 Track Progress—in a Process Led by Program Leadership—and React Quickly
3.1.3 Foster a Culture of Equity, Access, and Service; Not One of Preventing Fraud
3.2. Technical Recommendations
3.2.1 Simple Applications, Written in Plain Language and Informed by User Testing
3.2.2 Modern Online Application, with a Status Checker
3.2.3 Minimize the Information Required to Submit an Application
3.2.4 Accommodate Advance Claims
3.2.5 Follow Up by Phone or Email when Needed
3.2.6 (If relevant) Effect Smooth Transitions between Program Phases
3.2.7 Create a Beneficiary-centric Payment Delivery System
Of course the heart of the PFML program is its direct administration: how applications are submitted, how they are reviewed, and how efficient the whole process is. Again, while many of our findings are unique to New Jersey, other learnings are likely more generally applicable to other states.
Our findings here are split into two sections. First, we discuss several high-level conceptual and cultural considerations that impact the entire processing pipeline. Second, we discuss a series of more nuts-and-bolts measures that can make a meaningful difference in implementation. IT procurement and development are implicated in many of these points, but we discuss them separately, in the following section.
Recall throughout this section the point raised above: because it is a short-term program administered during major leave upheavals or crises for beneficiaries, PFML must be held to an especially high timeliness standard. Processing time must be measured in days or weeks, not months; and there is lower margin for error. (New Jersey aims to process applications in two weeks, which is a reasonable benchmark.) For a PFML program to be successful, it must excel in administration.
3.1. Conceptual and Cultural Considerations
3.1.1 Set Realistic Expectations and be Transparent
Beneficiaries appreciate transparency over ungrounded optimism. In the best case, all applications would be processed in under two weeks. Barring that, beneficiaries would rather know what to expect than be primed with unrealistic expectations that may not pan out.
This finding came up again and again in interviews. Official materials all indicated a two-week processing time, but, because of variance in the outcomes, beneficiaries had no faith in that estimate. This led stressed out applicants to repeatedly and futilely check their application status online, or inundate overworked agency call centers with status check queries. In some cases, the uncertainty was so severe that potential beneficiaries decided it was not worth applying at all:
I wish there was a better explanation of what happens after your application is submitted. I don’t know how long it will take to get paid… I’ve heard nightmares. – Interviewee #17
My husband wanted to [take bonding leave] but he couldn’t cause we didn’t know when we’d get the checks. They [DOL] said 2 weeks but when he talked to people [HR department, and friends], they said it came when it wanted. We can’t have that. It’s not worth the risk. That’s our house. – Interviewee #14
And, when applications took longer than two weeks, beneficiaries were generally bewildered:
“I wish they would have just denied me a lot quicker. If there is something wrong or they have to review something it takes an extra 5-6 weeks. Why does it take that long if it takes 14 days to review the whole application?” – Interviewee #18
The irony here is that, in fact, New Jersey was processing most applications in two to three weeks—but, a sizable minority took significantly longer, and, as bad news travels faster than good, these were the horror stories that people heard about. Without clear transparency about timelines, the public got the impression that long wait times are the norm, giving the program a worse reputation than it deserved.
First, program offices should be forthright about what goes on behind the scenes, and provide applicants with regular status updates. Second, and while it may cut against administrators’ instincts to keep potentially unsavory data under wraps, the program office has little to lose and much to gain from publicly posting data about its wait times. A simple way to do so is along the lines of: “90 percent of applications are paid or rejected within X days,” with X updated based on program data. This way beneficiaries know the outer limit of what they must wait through, in all but the most exceptional cases. (Note that reporting the average time to completion can be misleading. A mean could easily overstate the typical experience by including a few long outliers; but a median is equally misleading, as half of beneficiaries will be disappointed to see the process take longer than the number they read.) Such an approach would build trust with beneficiaries and allow them to plan appropriately.
From a program administrator’s perspective this approach could also be helpful in ensuring adequate program resources. If the average time to determination gets so large that it increases media and political attention, it can help administrators advocate compellingly for additional resources they need to improve wait times.
Recommendations:
- Explain clearly what goes on behind the scenes after an application is submitted.
- Provide regular updates on application status.
- Provide regularly updated and reliable estimates on current processing times.
3.1.2 Track Progress—In a Process Led by Program Leadership—and React Quickly
For administrators to share externally how long applications take, they must have clarity on this information internally as well. In a program where reliably quick processing is critical, administrators need robust, real-time visibility into the application processing pipeline.
This is easier said than done. This project is more complex than just knowing the average wait time, or, for example, the longest a given application has been sitting in the system. Administrators need information about the distribution of outcomes occurring in their programs; for example, a program where one half of applications are processed in one day and the other half in two months has an average wait time of one month, but that is very different from a program where every application takes one month to process. And, depending on how the program is set up, the specific outcomes that administrators must track to reliably make updates may differ.
Partly as a result, the largest hurdle to implementing such analysis in New Jersey—and likely in other environments as well—was not a lack of reporting or resources per se, but an inherited disconnect between the analytics department and the program leadership about what exactly needed to be measured. At NJDOL, significant resources had been devoted to TDI/FLI reporting, and the analytics department regularly delivered detailed and thorough statistics to program leadership—and had for decades. There was no lack of data. Rather, the data was simply not aggregated and presented in a way that program leadership could understand, or that answered all of their key questions.
Reporting and analytics can indeed be game-changing for program administrators, but only if done right. This means dynamic collaboration between leadership, with its program expertise, and the reporting team, with its data expertise, who can together decide which measures must be tracked and how they can be calculated.
As with the outreach data above, we offer an example of this analysis in New Jersey, not because the findings (or in this case even the research questions) will apply directly in other jurisdictions, but because the process itself is instructive of the type of findings that may emerge.
First, we performed a thorough review of the application process and application routing, talking not just to program leadership but to individual claim examiners and processors to understand how claims were being routed in practice under different circumstances. This step is critical; it is impossible to measure a process without knowing what it is, and even in government, processes frequently play out differently in real life than they do on paper. At a high level, in New Jersey, the process is:
- There is a separate backlog of applications for each of the four primary claim types, (TDI web, TDI paper, FLI web, FLI paper) with examiners all working on claims that are n days old depending on the length of the backlog (usually one to three weeks), and with examiners focused exclusively on either FLI or TDI claims.
- The first step for examiners working on paper claims is to enter them, which takes up to about half an hour; for web claims, this step is of course skipped.
- Once entered, examiners will review a claim, and can generally approve it very quickly if it is complete and correct; the approval can take as little as a few minutes. If the claim is missing information or otherwise problematic, examiners may either reject it immediately, or they may leave the claim open and try to resolve outstanding issues.
- Initially rejected claims frequently end up in a separate reconsideration unit, where processing is triggered by another category of forms submitted by applicants, each with their own backlogs.
Second, we reviewed in detail the existing application processing reports output by the mainframe, including sitting with reporting and analytics staff to understand which statistics they use, and what is represented by each number (a nontrivial task given that the decades-old reports are not clearly labeled, and any detailed documentation has been lost). We also checked each interpretation by comparing multiple different reports and highlighting and resolving any sources of discrepancy.
At the end of this process, we were able to perform a reliable analysis of the range of processing times for different applications. Again, these findings give examples of the kinds of things other jurisdictions might glean from a similar analysis. We found:
- Administrators had estimated that the average claim was probably taking as much as about one per month to process. In practice, though, there was a very wide distribution of processing times. A majority of claims were processed within the promised two to three weeks, but a significant portion stretched on much longer, with 10-20 percent of claims taking more than eight weeks. A better way to improve the user experience is to make the latter more like the former, rather than speed processing across the board.
- In an attempt to reach faster resolution, program administrators had been attempting to enforce a policy of quickly rejecting incomplete claims, and routing them to reconsideration, where staff can research further details as needed to resolve the claim. In practice, however, routing claims to reconsideration was highly counterproductive. Most claims going to the unit were ultimately granted, but the unit was relatively backlogged compared to others, and so granting them took up to an order of magnitude longer than handling them in the initial examination unit—a matter of months, rather than weeks.
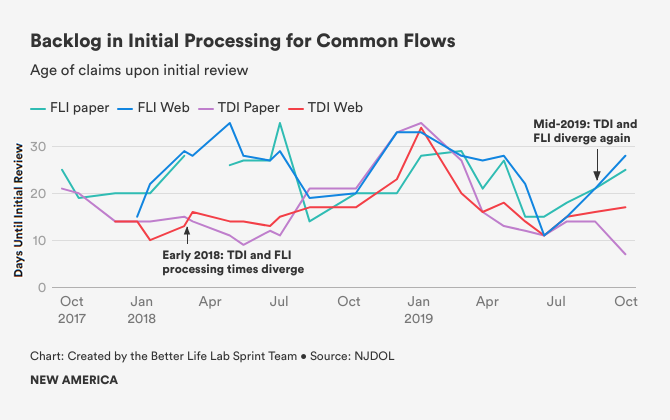
- Examiners’ rigid specialization in either TDI or FLI, rather than positively affecting economies of scale, was in fact likely hurting the program. Over the course of the previous months, there were periodic and unpredictable shifts in the volume of work coming in to the TDI and FLI programs. But because resources were not shifted between the two, wait times ballooned in one program then the other over time, with little done to keep the two waitlists concurrently in check. During the sprint, TDI claims were being reviewed within about one to two weeks, while FLI claims were taking up to a month.
- Almost all delays came from one of two sources: (a) the initial one to three week backlog, and (b) applications with incomplete data. Were it not for these factors, claims could be processed nearly instantly.
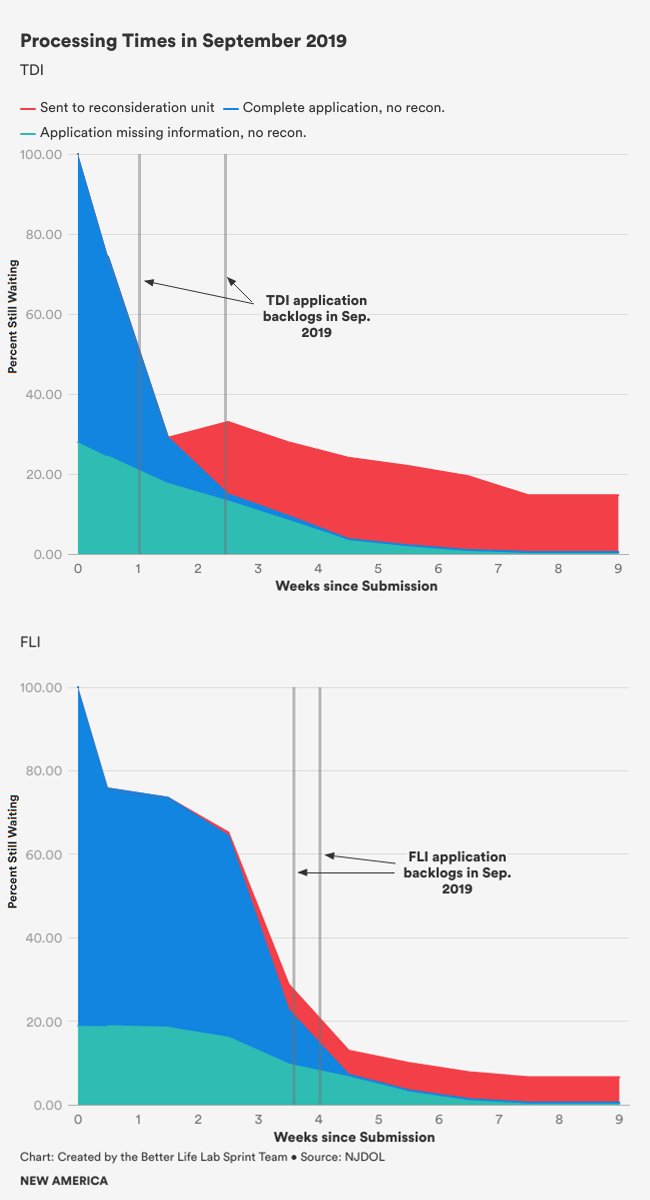
Ultimately, collaboratively producing a clear framework to analyze and understand the data, and working rigorously to measure the program’s progress through it, will help program offices learn what they need in order for the program to succeed.
Recommendations:
- PFML programs need real-time insight into how their application processing pipeline is working.
- The metrics programs track may depend on the details of their internal processes; analytics departments and program leadership should work collaboratively to develop the set of metrics that would be most helpful in tracking the applicant experience. As a rule of thumb, leadership should consider tracking:
- Portion of applications that are fully processed within two weeks (among applications submitted 2-6 weeks ago) — if applicable, broken out by application type
- Portion of applications that are fully processed within 30 days (among applications submitted 30-60 days ago) — if applicable, broken out by application type
- Current count of applications in each division’s work queue
- Portion of applications rejected, and, if applicable, reasons for rejection
- Program leadership should use the learnings from these analyses to set priorities and address delays, backlogs, and other issues as they arise.
3.1.3 Foster a Culture of Equity, Access, and Service; Not One of Preventing Fraud
In countless little decisions every day, program administrators must choose to err on the side of limiting the potential for fraud or increasing access. They should choose the latter, and do so clearly and unambiguously.
This choice plays out in obvious ways in the case of program-wide policy changes that the TDI/FLI leadership, to its significant credit, implemented in the last several years. A couple of examples illustrate the point:
- Claims that arrive later during the leave period require a valid reason for lateness outside the applicant’s control. But program leadership noticed that, in practice, many late applicants simply did not know about the program in time, often because their employers did not inform them. Rather than continue to punish these potential beneficiaries for the fact that no one told them about the program, the program chose to accept “my employer didn’t inform me of the program” as a valid reason for late claims.
- A common reason for delayed claim processing used to be minor mismatches in dates; a claimant wrote that their leave started on November 10, for instance, but their doctor wrote that it began on November 11. Previously, such claims were denied until the discrepancy could be resolved. Now, leadership’s guidance is to acknowledge that such mismatches are not actually evidence of a meaningful discrepancy, and to simply grant the claim.
It is important to foster this kind of understanding and empathetic workplace culture from top to bottom because front-line staff usually have discretion over numerous small decisions not visible to program leadership. An example from New Jersey: If an application came in without a required doctor’s note, the protocol was technically to reject the application out of hand, and to reopen processing in reconsideration if needed. But application examiners focused on getting to yes may have instead called the applicant, explained the situation, and found a way to get that note and grant the benefit. An office whose priority is inclusion will do this more frequently than an office that emphasizes zero tolerance for waste and fraud.
It is worth noting the relative difficulty of perpetrating a fraud in PFML programs—especially for parental leave. Not only would a would-be fraudster need to defraud the government, they would have to defraud their employer as well—or somehow manage to mislead the state about their legally-reported wages. And they would have to lie about life events that people are not generally inclined to lie about: as staff in New Jersey pointed out, how, and how frequently, does someone really fake having a child? For administrators, it is not simply that the risk of dissuading genuine applications is not worth the reward of weeding out a few fraudulent ones—it’s that there is in fact very little fraud to weed out at all.
Recommendations:
- Review program rules and restrictions, and remove those that serve to bar claimants from getting benefits without a commensurate benefit in weeding out true fraud.
- Communicate to employees the importance of inclusion, and, if applicable, ensure that performance criteria do not incentivize rejecting applications unnecessarily.
3.2. Technical Recommendations
The following recommendations are slightly more mechanical and detail-oriented, but still generic enough that they are likely to be broadly applicable to other states with PFML programs.
3.2.1 Simple Applications, Written in Plain Language and Informed by User Testing
The same guidance offered above with regards to program communications (Learning 1.4) applies with extra force on the development of an application. The application is the front door to a program, and if the program is to be accessible, the application must be as simple and straight-forward as humanly possible. Yet program staff can sometimes become mired in the minutiae of their program, and become unaware of their own blind spots when it comes to what potential applicants may find complex. The only reliable way to ensure a smooth process is to rigorously user-test the application with real claimants.
New Jersey’s experiences offer an illustration of the importance of user testing. Understanding the previous version could use improvement, TDI/FLI leadership undertook a significant overhaul of the program’s paper application in 2018, led by experienced program staff. The new application was far shorter than the previous one, and streamlined in powerful ways. But conversations with applicants and claim examiners during the sprint made clear that, while the overhaul had made very significant improvements, there were still some points of confusion. Examiners reported continuing to see frequent small errors: (1) claimants misrecorded the dates of leave submitted on claims, and (2) many claimants reported receiving Social Security Disability Insurance (SSDI) when they actually meant old-age Social Security, for example.
Two-thirds of our interviewees—some of whom used the older web application, which had not been recently updated and was widely acknowledged to be in worse shape than the paper one—had difficulty with the application. Many noted “guessing until they figured it out” when recording key dates, as they did not entirely understand what they were being asked: “I wasn’t sure about the stop date? I think they were looking for [the] last paid day [of work.] I figured it out by trial and error. I just kept guessing,” said Interviewee #5.1 Another mentioned that the application was not clear enough about the requirement to list all recent employers: “I didn’t add one employer because I didn’t work a lot of time with them. And then it stalled my application by 6 weeks. It wasn’t clear to add all employers,” and Interviewee #1.
There is no such thing as too simple or too streamlined in creating applications for benefits, and there is no substitute for testing the forms with a representative sample of real users. And, administrators should continue to monitor the applications that come in, looking for common errors and amending the application to prevent those mistakes.
3.2.2 Modern Online Application, with a Status Checker
A modern, well-tested, well-built, and well-designed web application—with functionality to submit and check the status of claims—is arguably the single greatest asset a program can have.
For one, most people expect to find government resources online, and strongly prefer online applications to legacy methods. (This is especially true for parental leave, where the user base is liable to skew younger.) In New Jersey, the paper (mail/fax) application is the legacy mainstay for many employers and community organizations, and is currently far more streamlined and easy to use than the web application; even so, the web application attracts 50 percent of applicants.
But, perhaps less obviously, web applications create enormous efficiency gains for the program, in multiple ways:
- Paper applications require manual data entry, which consumes a significant portion of claim examiners’ time; in New Jersey, processing a complete paper application took five to eight times longer than processing a complete web application.2
- Web applications can be validated and returned to users to correct errors before they are submitted. This is significant because incomplete claims accounted for a very large portion of delayed processing in New Jersey. Even with New Jersey’s imperfect web application, 87 percent of web claims were complete on receipt, compared with only 58 percent of paper claims, and web claims were only about a third as likely to get stuck in drawn-out determination processes.
- Claimants are understandably anxious about when their benefits will arrive and want regular updates. If they cannot do so online, they will seek the information some other way. In New Jersey, this phenomenon had played out in a major way: With an incomplete status check application inaccessible to many claimants, huge numbers of claimants instead called the department. These phone calls had, in turn, overwhelmed the call center, to the extent that every interviewee and program employee we spoke with cited call center traffic and delays as a major pain point in the application process.
A robust web application is not only a baseline expectation of customer service in the twenty-first century; it is also the simplest way to ease the pressure on other program divisions and improve efficiency. Note that the net result of these web improvements is not to remove humans from the process entirely, but rather to free up claim examiners and call center agents to provide useful services, rather than overwhelm them with purely clerical tasks.
As important as the web application is, it is important to keep in mind what it cannot do. A well-designed and sleek web application is no substitute for clear language that users can understand; in fact, using plain language on forms and testing them with users (as discussed in the previous section) is a prerequisite for developing a good web app. And, programs would be well-advised to maintain a paper form alongside the web application, for populations with connectivity issues.
More details about the design of a modern web app are described in the U.S. Web Design Standards. A few key points to keep in mind:
- Forms should be mobile responsive, as many Americans access the internet primarily or exclusively via smartphone. (One interviewee told us: “It was nice until I forgot my password. I couldn’t reset it because I was on a mobile device. I called, I waited a long time. When they told me I have to use a computer… I told them I don’t have one. They told me to go to the library. I have 7 kids. I can’t just get up and go.” -Interviewee #18)
- Forms should include a progress bar indicating to users how far along in the process they are, and should set clear expectations about how long sections will take.
- Forms should provide clarification about what exactly is being requested and why.
- Any personally identifiable information should be masked.
- Fields should be automatically validated, and return clear, actionable feedback where errors occur.
3.2.3 Minimize the Information Required to Submit an Application
Program administrators must resist the temptation to request every last piece of information that might be useful or interesting in application processing, program analysis, or audit readiness. Each additional piece of information requested is a potential barrier for prospective beneficiaries, and thus, critically, another source of delay in paying benefits. Administrators should source data on the back end where possible, and limit required documentation to the bare minimum.
New Jersey had taken several steps in this regard that bore dividends in improving access. A couple of examples:
- TDI/FLI used to require employers to submit records corroborating claimants’ wages, even though the state DOL necessarily has authoritative data on all wages paid in the state through the unemployment system. As this employer confirmation requirement was statutory, program leadership asked the state legislature to amend the law, and the legislature did so in early 2019. Now, staff rely entirely on the state’s system, and do not bog down employers’ HR departments compiling data that the government already has.
- FLI-Bonding claims—paid leave to bond with a newborn or newly adopted child—used to require formal documentation, for example a doctor’s note, akin to temporary disability claims. It became clear that the formality of getting a doctor to sign a letter that a baby was indeed born was a barrier for new parents who were understandably thinking about hundreds of other things before acquiring proof that their baby was indeed a baby. NJDOL administratively waived the documentation requirement for bonding claims.
It is impossible to estimate the quantitative effect of these changes on applications and approvals, but, anecdotally, they are significant for improving access, especially in a program where every added day and every added document matters.3 Our analysis found that the vast majority of processing delays came from applications that arrived incomplete, where additional information needed to be tracked down. Reducing the number of requirements mechanically decreases these delays. Administrators should always design their programs to minimize the onus placed on claimants, and their employers and doctors.
3.2.4 Accommodate Advance Claims
Some PFML users will have no advance warning, as in the case of a sudden illness or injury for them or a family member—but, frequently, beneficiaries can anticipate when they will need leave, and want to prepare. They know roughly when a baby will be born or when they or a family member has a scheduled surgery, and they want to prepare for it weeks in advance, rather than having to submit forms while in the hospital:
“Right after a baby, you’re a zombie. Will you remember to apply?” – Interviewee #1
“They didn’t want to talk to you until you were 60 days from the due date. I’m a planner; I wanted to talk sooner. It was stressful.” – Interviewee #8
As of late 2019, New Jersey partially allowed beneficiaries to file advance claims, but many interviewees reported confusion over how to do so. Programs should have a way for claimants to file most of a claim, and trigger it—with an absolute minimum of additional effort—when the moment is right. And programs should be able to review and provisionally approve these partial claims, so any issues can be worked out in advance.
3.2.5 Follow Up by Phone or Email when Needed
Well-designed web applications and streamlined lists of requirements should decrease the need for custom follow-up with individual applicants. Insofar as such follow-up is still necessary, though, in line with the spirit of prioritizing customer service over compliance, program staff should follow up with claimants via phone or email. In government, it is easy to default to mail notices, and indeed New Jersey’s program had historically done so, sending off form letters to claimants when there were issues in the application. Such letters—which are often imprecise and missing key information—waste several days in the mail in the best case scenario. Often, they waste weeks: The instructions are insufficient to correct the initial error and there is no way to get clarification from the department. Then, the applicant submits a second application that is equally flawed, and the whole process starts all over again. Examiners should make it easy for claimants to quickly correct issues so their applications can be processed.
Setting up policies like this can be slightly more complex than simply encouraging examiners to change their methods. In New Jersey, for example, many examiners did go above and beyond, calling or emailing claimants to quickly address issues. However, because they called or emailed from their direct lines or addresses, claimants frequently passed around that information to other friends with issues, recommending this contact as a quick way to resolve questions, to the point that the well-meaning examiner was inundated with extra work not their own. Examiners in this case need the ability to call or email from generic lines or addresses, like in any other customer service department. Another barrier is the exchange of personally identifiable information. New Jersey generally used Social Security Number as its key ID for applications, rather than an application ID. This practice of course raised challenges for examiners who (rightly) did not want to include such sensitive personally identifiable information in an email.
While these two barriers are perhaps unique to New Jersey’s specific system, it underscores the point that a good customer service solution to follow up with claimants must make it easier for examiners to do the right thing, not harder.
3.2.6 (If Relevant) Effect Smooth Transitions between Program Phases
As discussed, paid maternity leave beneficiaries in New Jersey are eligible for two different programs in succession: first, TDI for birthing parents to recover; second, FLI to bond with their new infant. Again, in the best case scenario, this would be one program that lasts for the full length of leave. Barring such a unification, though, the transition process from one type of leave to another must be incredibly seamless; new parents who think they have their benefits worked out are not in a position to navigate even relatively limited paperwork in the weeks immediately after childbirth.
New Jersey had made strides to “automate” these claims; there is a specific form for birthing parents transitioning from TDI to FLI, which is mailed to TDI beneficiaries pre-populated for them to send back. (Non-birthing parents, again, are not eligible for TDI leave.) This application, unlike other claims, did not have to be reviewed by a human at NJDOL. Even so, evidence suggested the process was still not simple enough. Multiple interviewees cited confusion over these so-called “transitional bonding” claims. Some were special cases (private plans covered the TDI portion of the leave, and they were switching to the public plan for the second portion), and some were confused because they had not been told what to expect. And, as discussed earlier, the curious divergence between TDI and FLI usage suggests this issue may have been more widespread still, with perhaps as many as half of birthing parents failing to transition to FLI when they could indeed do so.
3.2.7 Create a Beneficiary-centric Payment Delivery System
Like other DOL programs in a variety of states, TDI/FLI payments were delivered exclusively via a prepaid Bank of America (BoA) debit card. Making payments available via debit card for the meaningful fraction of Americans who are unbanked is a useful step in the name of accessibility, and states should offer the option when possible.4 But the default option—especially for a population that is formally employed, and thus likely to be banked—should be direct deposit; anything else is another unnecessary point of friction between claimants and their benefits.
Insofar as administrators pursue debit cards for PFML programs, there are a couple of points to keep in mind. First, while debit cards pose no structural issues for delivering long-term benefits like Social Security, the timeliness of PFML benefits poses a serious challenge. Even in the best case scenario, issuing a debit card generally takes a few days, since the card has to arrive in the mail, on top of whatever processing time is required at the bank. New Jersey eliminates this wait time by issuing the cards as soon as applications are received, whether or not the claim is approved, so that claimants have the card in hand if and when their benefits are approved. But this creative workaround caused confusion too, with claimants discarding the unmarked mystery cards when they arrived in the mail prior to the benefit approval notice, or with claimants unsure how to know when the benefits had been loaded onto the card. Given how long they take to issue (and the confusion created by workarounds), debit cards are simply not a great solution for programs with short time scales.
Second, implementation details matter, and the BoA contract, in the details, created trouble for beneficiaries. Under the terms of the contract New Jersey and BoA negotiated, the cards remained valid for several years and across any NJDOL program—meaning that if someone used unemployment benefits in 2017, their TDI/FLI benefits in 2019 would be sent to the same card. If the beneficiary had disposed of their card after moving off unemployment, they had to pay a fee for a new card. If beneficiaries had challenges with the cards they were referred to BoA customer service and the department had limited controls on response time and customer service after the hand-off.
We offer this caution, though, to new programs—the payment system can have significant long-term consequences for both users and state employees. Choose your contracts wisely and create terms that allow you to improve and measure customer service.
Citations
- Interviewee #8: “The wording for the dates was weird.”
- Examiners reported that it takes two minutes to approve a complete claim, and 10-15 minutes to manually enter data from a paper claim.
- Anecdotally, we were told that when the department announced the change about wage documentation at an employer association meeting, they got a standing ovation from the HR managers in attendance.
- DirectExpress also proves that benefits delivered via debit card can work at scale; source
